I Had Neutropenia When I Was a Baby. Can It Happen Again?
Neutropenia is a reduction in the claret neutrophil count. If information technology is severe, the risk and severity of bacterial and fungal infections increase. Focal symptoms of infection may be muted, but fever is present during most serious infections. Diagnosis is by white blood cell count with differential, and evaluation requires identification of the crusade. If fever is present, infection is presumed, and firsthand, empiric broad-spectrum antibiotics are necessary, especially if the neutropenia is severe. Treatment with granulocyte colony-stimulating factor is sometimes helpful.
The normal lower limit of the neutrophil count (total white blood cell count × % neutrophils and bands) is 1500/mcL (1.5 × 109/50) in whites and is somewhat lower in blacks (about 1200/mcL [one.ii × 109/L). Neutrophil counts are not equally stable every bit other prison cell counts and may vary considerably over brusk periods, depending on many factors such as activity condition, anxiety, infections, and drugs. Thus, several measurements may exist needed when determining the severity of neutropenia.
Severity of neutropenia relates to the relative risk of infection and is classified as follows:
-
Balmy: m to 1500/mcL (1 to 1.5 × 10nine/L)
-
Moderate: 500 to 1000/mcL (0.5 to i × 109/L)
-
Severe: < 500/mcL (< 0.v × 109/50)
When neutrophil counts autumn to < 500/mcL, endogenous microbial flora (eg, in the rima oris or gut) tin cause infections. If the count falls to < 200/mcL (< 0.2 × 109/Fifty), the inflammatory response may be muted and the usual inflammatory findings of leukocytosis or white claret cells in the urine or at the site of infection may non occur. Acute, astringent neutropenia, particularly if another factor (eg, cancer) is present, significantly impairs the immune arrangement and tin can lead to rapidly fatal infections. The integrity of the skin and mucous membranes, the vascular supply to tissue, and the nutritional status of the patient also influence the risk of infections.
The virtually ofttimes occurring infections in patients with profound neutropenia are
Vascular catheters and other puncture sites confer extra run a risk of pare infections; the virtually common bacterial causes are coagulase-negative staphylococci and Staphylococcus aureus, just other gram-positive and gram-negative infections also occur. Stomatitis Stomatitis Oral inflammation and ulcers, known as stomatitis, may be mild and localized or astringent and widespread. They are invariably painful. (See also Evaluation of the Dental Patient and Gingivitis... read more than 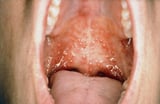 , gingivitis Gingivitis Gingivitis is a type of periodontal disease characterized by inflammation of the gums (gingivae), causing bleeding with swelling, redness, exudate, a alter of normal contours, and, occasionally... read more
, gingivitis Gingivitis Gingivitis is a type of periodontal disease characterized by inflammation of the gums (gingivae), causing bleeding with swelling, redness, exudate, a alter of normal contours, and, occasionally... read more 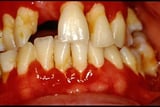 , perirectal inflammation, colitis, sinusitis Sinusitis Sinusitis is inflammation of the paranasal sinuses due to viral, bacterial, or fungal infections or allergic reactions. Symptoms include nasal obstruction and congestion, purulent rhinorrhea... read more than
, perirectal inflammation, colitis, sinusitis Sinusitis Sinusitis is inflammation of the paranasal sinuses due to viral, bacterial, or fungal infections or allergic reactions. Symptoms include nasal obstruction and congestion, purulent rhinorrhea... read more than  , paronychia Acute Paronychia Paronychia is infection of the periungual tissues. Astute paronychia causes redness, warmth, and pain along the nail margin. Diagnosis is by inspection. Treatment is with antistaphylococcal antibiotics... read more
, paronychia Acute Paronychia Paronychia is infection of the periungual tissues. Astute paronychia causes redness, warmth, and pain along the nail margin. Diagnosis is by inspection. Treatment is with antistaphylococcal antibiotics... read more 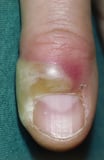 , and otitis media Otitis Media (Acute) Acute otitis media is a bacterial or viral infection of the heart ear, commonly accompanying an upper respiratory infection. Symptoms include otalgia, frequently with systemic symptoms (eg, fever... read more
, and otitis media Otitis Media (Acute) Acute otitis media is a bacterial or viral infection of the heart ear, commonly accompanying an upper respiratory infection. Symptoms include otalgia, frequently with systemic symptoms (eg, fever... read more 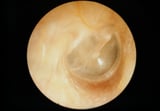 ofttimes occur. Patients with prolonged neutropenia later on hematopoietic stem cell transplantation or chemotherapy and patients receiving loftier doses of corticosteroids are predisposed to fungal infections.
ofttimes occur. Patients with prolonged neutropenia later on hematopoietic stem cell transplantation or chemotherapy and patients receiving loftier doses of corticosteroids are predisposed to fungal infections.
Acute neutropenia (occurring over hours to a few days) can develop as a result of
-
Rapid neutrophil use or destruction
-
Impaired production
Chronic neutropenia (lasting months to years) usually arises as a result of
-
Reduced product
-
Excessive splenic sequestration
Neutropenia also may exist classified as
-
Principal due to an intrinsic defect in marrow myeloid cells
-
Secondary due to factors extrinsic to marrow myeloid cells
Neutropenia caused by intrinsic defects in myeloid cells or their precursors is uncommon, but when present, the nigh common causes include
-
Chronic idiopathic neutropenia
-
Congenital neutropenia
Chronic benign neutropenia is a blazon of chronic idiopathic neutropenia in which the rest of the allowed system appears to remain intact; even with neutrophil counts < 200/mcL (< 0.ii × 10nine/L), serious infections usually do not occur, probably because neutrophils are sometimes produced in adequate quantities in response to infection. It is more mutual in women.
Severe congenital neutropenia (SCN, or Kostmann syndrome) is a heterogenous grouping of rare disorders that are characterized past an abort in myeloid maturation at the promyelocyte stage in the os marrow, resulting in an absolute neutrophil count of < 200/mcL and significant infections starting in infancy. SCN tin can exist autosomal ascendant or recessive, X-linked, or sporadic. Several genetic abnormalities that cause SCN have been identified, including mutations affecting neutrophil elastase (ELANE/ELA2), HAX1, GFI1, and the One thousand-CSF (granulocyte colony-stimulating factor) receptor (CSF3R). Almost patients with SCN will answer to chronic growth factor therapy, just hematopoietic stalk cell transplantation Hematopoietic Stalk Cell Transplantation Hematopoietic stalk cell (HSC) transplantation is a apace evolving technique that offers a potential cure for hematologic cancers (leukemias, lymphomas, myeloma) and other hematologic disorders... read more may demand to be considered for poor responders. SCN patients accept an increased risk of developing myelodysplasia Myelodysplastic Syndrome (MDS) The myelodysplastic syndrome (MDS) is group of disorders typified by peripheral cytopenia, dysplastic hematopoietic progenitors, a hypercellular or hypocellular bone marrow, and a high chance... read more or acute myeloid leukemia Acute Myeloid Leukemia (AML) In acute myeloid leukemia (AML), malignant transformation and uncontrolled proliferation of an abnormally differentiated, long-lived myeloid progenitor cell results in high circulating numbers... read more  .
.
Circadian neutropenia is a rare congenital granulocytopoietic disorder, commonly transmitted in an autosomal dominant way and usually caused past a mutation in the gene for neutrophil elastase (ELANE/ELA2), resulting in abnormal apoptosis. It is characterized by regular, periodic oscillations in the number of peripheral neutrophils. The mean oscillatory menstruation is 21 ± three days. Cycling of other claret cells is also evident in most cases.
Beneficial ethnic neutropenia occurs in members of some indigenous groups (eg, some people of African, Middle Eastern, and Jewish descent). They normally have lower neutrophil counts but practice not have increased risk of infection. In some cases this finding has been linked to the Duffy red blood cell antigen; some experts retrieve neutropenia in these populations is related to protection from malaria Malaria Malaria is infection with Plasmodium species. Symptoms and signs include fever (which may be periodic), chills, rigors, sweating, diarrhea, abdominal pain, respiratory distress, confusion... read more than .
Neutropenia can likewise result from os marrow failure due to rare congenital syndromes (eg, cartilage-hair hypoplasia syndrome, Chédiak-Higashi syndrome Chédiak-Higashi Syndrome Chédiak-Higashi syndrome is a rare, autosomal recessive syndrome characterized by impaired lysis of phagocytized leaner, resulting in recurrent bacterial respiratory and other infections... read more than , dyskeratosis congenita, glycogen storage disease type IB, Shwachman-Diamond syndrome, warts, hypogammaglobulinemia, infections, myelokathexis [WHIM] syndrome). Neutropenia is also a characteristic of myelodysplasia Myelodysplastic Syndrome (MDS) The myelodysplastic syndrome (MDS) is group of disorders typified by peripheral cytopenia, dysplastic hematopoietic progenitors, a hypercellular or hypocellular bone marrow, and a high risk... read more , where information technology may exist accompanied by megaloblastoid features in the bone marrow, and of aplastic anemia Aplastic Anemia Aplastic anemia is a disorder of the hematopoietic stalk cell that results in a loss of blood prison cell precursors, hypoplasia or aplasia of bone marrow, and cytopenias in two or more jail cell lines ... read more  and can occur in dysgammaglobulinemia and paroxysmal nocturnal hemoglobinemia Paroxysmal Nocturnal Hemoglobinuria (PNH) Paroxysmal nocturnal hemoglobinuria (PNH) is a rare acquired disorder characterized by intravascular hemolysis and hemoglobinuria. Leukopenia, thrombocytopenia, arterial and venous thromboses... read more .
and can occur in dysgammaglobulinemia and paroxysmal nocturnal hemoglobinemia Paroxysmal Nocturnal Hemoglobinuria (PNH) Paroxysmal nocturnal hemoglobinuria (PNH) is a rare acquired disorder characterized by intravascular hemolysis and hemoglobinuria. Leukopenia, thrombocytopenia, arterial and venous thromboses... read more .
Secondary neutropenia can result from utilize of certain drugs, bone marrow infiltration or replacement, certain infections, or immune reactions.
The nearly mutual causes include
-
Drugs
-
Infections and immune reactions
-
Marrow infiltrative processes
Drug-induced neutropenia is one of the nigh common causes of neutropenia. Drugs tin can decrease neutrophil production through toxic, idiosyncratic, or hypersensitivity mechanisms; or they can increase peripheral neutrophil destruction through immune mechanisms. Only the toxic mechanism (eg, with phenothiazines) causes dose-related neutropenia.
Severe dose-related neutropenia occurs predictably after cytotoxic cancer drugs or radiation therapy due to suppression of bone marrow production.
Idiosyncratic reactions are unpredictable and occur with a broad variety of drugs, including alternative medicine preparations or extracts, and toxins.
Hypersensitivity reactions Drug Hypersensitivity Drug hypersensitivity is an allowed-mediated reaction to a drug. Symptoms range from mild to severe and include rash, anaphylaxis, and serum sickness. Diagnosis is clinical; skin testing is occasionally... read more are rare and occasionally involve antiseizure drugs (eg, phenytoin, phenobarbital), methimazole, or propylthiouracil. These reactions may final for only a few days or for months or years. Often, hepatitis Overview of Acute Viral Hepatitis Acute viral hepatitis is diffuse liver inflammation caused past specific hepatotropic viruses that accept diverse modes of transmission and epidemiologies. A nonspecific viral prodrome is followed... read more than , nephritis, pneumonitis, or aplastic anemia Aplastic Anemia Aplastic anemia is a disorder of the hematopoietic stem cell that results in a loss of blood jail cell precursors, hypoplasia or aplasia of bone marrow, and cytopenias in 2 or more cell lines ... read more  accompanies hypersensitivity-induced neutropenia.
accompanies hypersensitivity-induced neutropenia.
Immune-mediated drug-induced neutropenia, thought to ascend from drugs that act as haptens to stimulate antibody formation, usually persists for about 1 week after the drug is stopped. Information technology may result from aminopyrine, clozapine, propylthiouracil and other antithyroid drugs, penicillin, or other antibiotics.
Allowed defects can cause neutropenia. Neonatal isoimmune neutropenia can occur with fetal/maternal neutrophil antigen incompatibility associated with transplacental transfer of IgG antibodies against the newborn's neutrophils (most commonly to HNA-1 antigens). Autoimmune neutropenia can occur at any age and may be operative in many cases of idiopathic chronic neutropenia. Testing for antineutrophil antibodies (immunofluorescence, agglutination, or menstruum cytometry) is not always available or reliable.
Chronic secondary neutropenia often accompanies HIV infection Human being Immunodeficiency Virus (HIV) Infection Human immunodeficiency virus (HIV) infection results from 1 of 2 similar retroviruses (HIV-1 and HIV-2) that destroy CD4+ lymphocytes and impair cell-mediated immunity, increasing risk of certain... read more  considering of dumb product of neutrophils and accelerated destruction of neutrophils by antibodies. Autoimmune neutropenias may be astute, chronic, or episodic. They may involve antibodies directed against circulating neutrophils or neutrophil precursor cells. They may also involve cytokines (eg, gamma interferon, tumor necrosis factor) that can cause neutrophil apoptosis. Most patients with autoimmune neutropenia have an underlying autoimmune disorder or lymphoproliferative disorder (eg, large granular lymphocyte [LGL syndrome [a clonal disease of large granular lymphocytes], systemic lupus erythematosus Systemic Lupus Erythematosus (SLE) Systemic lupus erythematosus is a chronic, multisystem, inflammatory disorder of autoimmune etiology, occurring predominantly in young women. Common manifestations may include arthralgias and... read more
considering of dumb product of neutrophils and accelerated destruction of neutrophils by antibodies. Autoimmune neutropenias may be astute, chronic, or episodic. They may involve antibodies directed against circulating neutrophils or neutrophil precursor cells. They may also involve cytokines (eg, gamma interferon, tumor necrosis factor) that can cause neutrophil apoptosis. Most patients with autoimmune neutropenia have an underlying autoimmune disorder or lymphoproliferative disorder (eg, large granular lymphocyte [LGL syndrome [a clonal disease of large granular lymphocytes], systemic lupus erythematosus Systemic Lupus Erythematosus (SLE) Systemic lupus erythematosus is a chronic, multisystem, inflammatory disorder of autoimmune etiology, occurring predominantly in young women. Common manifestations may include arthralgias and... read more  , Felty syndrome).
, Felty syndrome).
Symptoms and Signs of Neutropenia
Neutropenia is asymptomatic until infection develops. Fever is ofttimes the simply indication of infection. If neutropenia is astringent, typical signs of focal inflammation (erythema, swelling, hurting, infiltrates) may be muted or absent. Focal symptoms (eg, oral ulcers) may develop but are often subtle. Patients with drug-induced neutropenia due to hypersensitivity may have a fever, rash, and lymphadenopathy equally a result of the hypersensitivity.
Some patients with chronic beneficial neutropenia and neutrophil counts < 200/mcL (< 0.2 × 109/L) practice not experience many serious infections. Patients with cyclic neutropenia or severe built neutropenia tend to have episodes of oral ulcers, stomatitis, or pharyngitis and lymph node enlargement during severe neutropenia. Pneumonias and septicemia often occur.
-
Clinical suspicion (repeated or unusual infections)
-
Confirmatory consummate claret count (CBC) with differential
-
Evaluation for infection with cultures and imaging
-
Identification of machinery and cause of neutropenia
Neutropenia is suspected in patients with frequent, severe, or unusual infections or in patients at risk (eg, those receiving cytotoxic drugs or radiation therapy). Confirmation is by CBC with differential.
The kickoff priority is to determine whether an infection is present. Because infection may be subtle, concrete examination systematically assesses the well-nigh mutual main sites of infection: mucosal surfaces, such as the alimentary tract (gums, pharynx, anus); lungs; abdomen; urinary tract; skin and fingernails; venipuncture sites; and vascular catheters.
If neutropenia is astute or severe, laboratory evaluation must proceed chop-chop.
Cultures are the mainstay of evaluation. At least 2 sets of bacterial and fungal blood cultures are obtained from all febrile patients; if an indwelling IV catheter is present, cultures are drawn from the catheter and from a separate peripheral vein. Persistent or chronic drainage material is likewise cultured for leaner, fungi, and atypical mycobacteria. Mucosal ulcers are swabbed and cultured for herpes virus and Candida. Skin lesions are aspirated or biopsied for cytology and civilization. Samples for urinalysis and urine cultures are obtained from all patients. If diarrhea is present, stool is evaluated for enteric bacterial pathogens and Clostridioides (formerly Clostridium) difficile toxins. Sputum cultures are obtained to evaluate for pulmonary infections.
Imaging studies are helpful. Chest ten-rays are done on all patients. A chest CT may also be necessary in immunosuppressed patients. CT of the paranasal sinuses may be helpful if symptoms or signs of sinusitis (eg, positional headache, upper molar or maxillary pain, facial swelling, nasal discharge) are present. CT scan of the abdomen is normally washed if symptoms (eg, hurting) or history (eg, contempo surgery) suggests an intra-abdominal infection.
Side by side, mechanism and cause of neutropenia are determined. The history addresses family history, presence of other disorders, all drugs, other preparations, and possible toxin exposure or ingestion.
If no obvious crusade is identified (eg, chemotherapy), the well-nigh important test is
-
Bone marrow examination
Bone marrow examination determines whether neutropenia is due to decreased marrow production or is secondary to increased prison cell destruction (determined by normal or increased production of the myeloid cells). Bone marrow examination may likewise indicate the specific cause of the neutropenia (eg, aplastic anemia Aplastic Anemia Aplastic anemia is a disorder of the hematopoietic stem cell that results in a loss of claret cell precursors, hypoplasia or aplasia of bone marrow, and cytopenias in two or more cell lines ... read more  , myelofibrosis Primary Myelofibrosis Main myelofibrosis (PMF) is a chronic myeloproliferative neoplasm characterized by bone marrow fibrosis, splenomegaly, and anemia with nucleated and teardrop-shaped reddish blood cells. Diagnosis... read more , myelodysplastic disorder Myelodysplastic Syndrome (MDS) The myelodysplastic syndrome (MDS) is grouping of disorders typified by peripheral cytopenia, dysplastic hematopoietic progenitors, a hypercellular or hypocellular bone marrow, and a high take a chance... read more , leukemia Overview of Leukemia Leukemia is a malignant condition involving the backlog product of immature or aberrant leukocytes, which eventually suppresses the production of normal claret cells and results in symptoms... read more ). Additional marrow studies (eg, cytogenetic analysis; special stains and flow cytometry for detecting leukemia, other malignant disorders, and infections) are washed.
, myelofibrosis Primary Myelofibrosis Main myelofibrosis (PMF) is a chronic myeloproliferative neoplasm characterized by bone marrow fibrosis, splenomegaly, and anemia with nucleated and teardrop-shaped reddish blood cells. Diagnosis... read more , myelodysplastic disorder Myelodysplastic Syndrome (MDS) The myelodysplastic syndrome (MDS) is grouping of disorders typified by peripheral cytopenia, dysplastic hematopoietic progenitors, a hypercellular or hypocellular bone marrow, and a high take a chance... read more , leukemia Overview of Leukemia Leukemia is a malignant condition involving the backlog product of immature or aberrant leukocytes, which eventually suppresses the production of normal claret cells and results in symptoms... read more ). Additional marrow studies (eg, cytogenetic analysis; special stains and flow cytometry for detecting leukemia, other malignant disorders, and infections) are washed.
Farther testing, such as flow cytometry and T-cell receptor gene rearrangement for the LGL syndrome, may be needed to determine the cause of neutropenia, depending on the diagnoses suspected. In patients at risk of nutritional deficiencies, levels of copper Acquired Copper Deficiency Copper is a component of many trunk proteins; almost all of the body's copper is bound to copper proteins. Copper deficiency may be acquired or inherited. (See besides Overview of Mineral Deficiency... read more , folate Folate Deficiency Folate deficiency is mutual. It may result from inadequate intake, malabsorption, or utilise of various drugs. Deficiency causes megaloblastic anemia (indistinguishable from that due to vitamin... read more , and vitamin B12 Vitamin B12 Deficiency Dietary vitamin B12 deficiency commonly results from inadequate absorption, merely deficiency can develop in vegans who practice not take vitamin supplements. Deficiency causes megaloblastic anemia, damage... read more are determined. Testing for the presence of antineutrophil antibodies is done if immune neutropenia is suspected. Differentiation between neutropenia caused past sure antibiotics and infection can sometimes be hard. The white blood cell count only before the start of antibiotic handling usually reflects the change in blood count due to the infection.
Patients who have had chronic neutropenia since infancy and a history of recurrent fevers and chronic gingivitis should have white cell counts with differential done three times/week for 6 weeks, and so that periodicity suggestive of circadian neutropenia can be evaluated. Platelet and reticulocyte counts are done simultaneously. In patients with cyclic neutropenia, eosinophils, reticulocytes, and platelets oft cycle synchronously with the neutrophils, whereas monocytes and lymphocytes may bike out of stage.
Molecular genetic testing for ELANE and other genes is advisable when congenital causes are considered.
-
Treatment of associated atmospheric condition (eg, infections, stomatitis)
-
Sometimes antibiotic prophylaxis
-
Myeloid growth factors
-
Discontinuation of suspected etiologic agent (eg, drug)
-
Sometimes corticosteroids
Suspected infections are always treated immediately. If fever or hypotension is present, serious infection is assumed, and empiric, high-dose, broad-spectrum antibiotics are given IV. Regimen option is based on the nearly likely infecting organisms, the antimicrobial susceptibility of pathogens at that particular institution, and the regimen'southward potential toxicity. Because of the risk of creating resistant organisms, vancomycin is used only if gram-positive organisms resistant to other drugs are suspected.
Indwelling vascular catheters can ordinarily remain in identify even if bacteremia is suspected or documented, but removal is considered if infections involve S. aureus, Bacillus, Corynebacterium, or Candida or another mucus or if blood cultures are persistently positive despite advisable antibiotics. Infections caused past coagulase-negative staphylococci mostly resolve with antimicrobial therapy alone. Indwelling Foley catheters tin too predispose to infections in neutropenic patients, and change or removal of the catheter should exist considered for persistent urinary infections.
If cultures are positive, antibiotic therapy is adjusted to the results of sensitivity tests. If a patient defervesces within 72 hours, antibiotics are connected for at least vii days and until the patient has no symptoms or signs of infection. When neutropenia is transient (such as that following myelosuppressive chemotherapy), antibiotic therapy is normally continued until the neutrophil count is > 500/mcL (> 0.5 × ten9/L); nevertheless, stopping antimicrobials tin be considered in selected patients with persistent neutropenia, especially those in whom symptoms and signs of inflammation accept resolved, if cultures remain negative.
Fever that persists > 72 hours despite antibiotic therapy suggests
-
A nonbacterial cause
-
Infection with a resistant species
-
Superinfection with a 2nd bacterial species
-
Inadequate serum or tissue levels of the antibiotics
-
Localized infection, such every bit an abscess
Neutropenic patients with persistent fever are reassessed every ii to 4 days with physical examination, cultures, and chest x-ray. If the patient is well except for the presence of fever, the initial antibody regimen tin exist continued, and drug-induced fever should exist considered. If the patient is deteriorating, alteration of the antimicrobial regimen is considered.
For afebrile patients with neutropenia, antibody prophylaxis can be considered although alterations in the bacterial microbiome may slow bone marrow recovery (one Treatment reference Neutropenia is a reduction in the blood neutrophil count. If it is severe, the risk and severity of bacterial and fungal infections increase. Focal symptoms of infection may be muted, but fever... read more ). Treatment with fluoroquinolones (levofloxacin, ciprofloxacin) is used in some centers for patients who receive chemotherapy regimens that commonly consequence in neutrophils ≤ 100/mcL (≤ 0.one × 109/L) for > 7 days. Prophylaxis is usually started by the treating oncologist. Antibiotics are connected until the neutrophil count increases to > 1500/mcL (> 1.5 × 109/L). Also, antifungal therapy tin can be given for afebrile neutropenic patients at higher risk of fungal infection (eg, after hematopoietic stem cell transplantation Hematopoietic Stem Cell Transplantation Hematopoietic stem jail cell (HSC) transplantation is a rapidly evolving technique that offers a potential cure for hematologic cancers (leukemias, lymphomas, myeloma) and other hematologic disorders... read more , intensive chemotherapy for acute myeloid leukemia Astute Myeloid Leukemia (AML) In acute myeloid leukemia (AML), malignant transformation and uncontrolled proliferation of an abnormally differentiated, long-lived myeloid progenitor cell results in high circulating numbers... read more  or a myelodysplastic disorder Myelodysplastic Syndrome (MDS) The myelodysplastic syndrome (MDS) is grouping of disorders typified by peripheral cytopenia, dysplastic hematopoietic progenitors, a hypercellular or hypocellular bone marrow, and a high risk... read more than , prior fungal infections). Selection of the specific antifungal drug should exist guided by an communicable diseases specialist. Antibiotic and antifungal prophylaxis is not routinely recommended for afebrile neutropenic patients without risk factors who are anticipated to remain neutropenic for < 7 days on the basis of their specific chemotherapy regimen.
or a myelodysplastic disorder Myelodysplastic Syndrome (MDS) The myelodysplastic syndrome (MDS) is grouping of disorders typified by peripheral cytopenia, dysplastic hematopoietic progenitors, a hypercellular or hypocellular bone marrow, and a high risk... read more than , prior fungal infections). Selection of the specific antifungal drug should exist guided by an communicable diseases specialist. Antibiotic and antifungal prophylaxis is not routinely recommended for afebrile neutropenic patients without risk factors who are anticipated to remain neutropenic for < 7 days on the basis of their specific chemotherapy regimen.
Myeloid growth factors (ie, granulocyte colony-stimulating factor [Thousand-CSF]) are widely used to increment the neutrophil count and to prevent infections in patients with severe neutropenia (eg, after hematopoietic stem cell transplantation and intensive cancer chemotherapy). They are expensive. All the same, if the chance of febrile neutropenia is ≥ thirty% (as assessed by neutrophil count < 500 mcL [< 0.5 × x9/L], presence of infection during a previous cycle of chemotherapy, associated comorbid disease, or historic period > 75), growth factors are indicated. In full general, most clinical benefit occurs when the growth gene is administered beginning almost 24 hours subsequently completion of chemotherapy. Patients with neutropenia caused by an idiosyncratic drug reaction may also do good from myeloid growth factors, particularly if a delayed recovery is anticipated. The dose for G-CSF (filgrastim) is 5 to ten mcg/kg subcutaneously once a twenty-four hour period, and the dose for pegylated K-CSF (pegfilgrastim) is 6 mg subcutaneously once per chemotherapy cycle.
Glucocorticoids, anabolic steroids, and vitamins practice not stimulate neutrophil production but tin affect distribution and destruction. If acute neutropenia is suspected to be drug- or toxin-induced, all potentially etiologic agents are stopped. If neutropenia develops during handling with a drug known to induce low counts (eg, chloramphenicol), and so switching to an alternative antibiotic may be helpful.
Saline or hydrogen peroxide gargles every few hours, liquid oral rinses (containing viscous lidocaine, diphenhydramine, and liquid antacid), anesthetic lozenges (benzocaine xv mg every 3 or 4 hours), or chlorhexidine mouth rinses (ane% solution) twice a mean solar day or 3 times a twenty-four hours may relieve the discomfort of stomatitis with oropharyngeal ulcerations. Oral or esophageal candidiasis is treated with nystatin (400,000 to 600,000 units oral rinse 4 times a day; swallowed if esophagitis is nowadays), clotrimazole troche (10 mg slowly dissolved in the mouth 5 times a day), or systemic antifungal drugs (eg, fluconazole). A semisolid or liquid nutrition may be necessary during astute stomatitis or esophagitis, and topical analgesics (eg,viscous lidocaine) may be needed to minimize discomfort.
In some patients with accelerated neutrophil destruction acquired past autoimmune disorders, corticosteroids (generally, prednisone 0.5 to 1.0 mg/kg orally once a day) can increase blood neutrophils. This increase often tin can be maintained with alternating-mean solar day Chiliad-CSF therapy.
Splenectomy has been used in the past to increase the neutrophil count in some patients with splenomegaly and splenic sequestration of neutrophils (eg, Felty syndrome); yet, because growth factors and other newer therapies are oftentimes effective, splenectomy should exist avoided in most patients. Splenectomy can be considered for patients with persistent painful splenomegaly or with astringent neutropenia (ie, < 500/mcL [< 0.5 × x9/50]) and serious problems with infections in whom other treatments take failed. Patients should be vaccinated confronting infections acquired by Streptococcus pneumoniae, Neisseria meningitidis, and Haemophilus influenzae before splenectomy because splenectomy predisposes patients to infection by encapsulated organisms.
-
1. Yan H, Baldridge MT, Yang KY: Hematopoiesis and the bacterial microbiome. Blood 132: 559–564, 2018. doi: x.1182/claret-2018-02-832519
-
Neutropenia predisposes to bacterial and fungal infections.
-
The chance of infection is proportional to the severity of neutropenia; patients with neutrophil counts < 500/mcL (< 0.v × 109/L) are at greatest chance.
-
Considering the inflammatory response is express, clinical findings may exist muted, although fever is usually nowadays.
-
Delirious neutropenic patients are treated empirically with broad-spectrum antibiotics awaiting definitive identification of infection.
-
Antibiotic prophylaxis may be indicated in high-run a risk patients.
wagneraboverpured.blogspot.com
Source: https://www.msdmanuals.com/professional/hematology-and-oncology/leukopenias/neutropenia
0 Response to "I Had Neutropenia When I Was a Baby. Can It Happen Again?"
Post a Comment